- Mar 24
Understanding PMS and the keys to heal naturally
- Shabina
- Menstrual Cycle
- 0 comments
We've all been there: a few days before your period, everything feels harder — the cramps, the mood swings, the bottomless craving for chocolate, the inexplicable urge to cry during a cereal commercial. Sound familiar?
These symptoms aren't just part of "being a woman." They're signs of something called Premenstrual Syndrome (PMS) — and understanding it is the first step to feeling better.

What exactly is PMS?
Premenstrual Syndrome (PMS) refers to a recurring set of physical and psychological symptoms that appear in the days before your period and typically disappear within hours of it starting. It can begin as early as right after ovulation — up to two weeks before menstruation.
PMS affects between 20 and 40% of people with periods. While some level of pre-period discomfort is normal (mild fatigue, a little bloating, slight cramps), symptoms severe enough to interfere with daily life are not just a fact of life — they signal an underlying imbalance worth addressing.

The symptoms of PMS
Specialists have catalogued over 150 symptoms linked to PMS. Here are the most common, split into two categories:
Your cycle in four phases
To understand PMS, you need to understand your cycle. It's not just "the week you bleed" — it's a four-phase hormonal journey governed by four key hormones: FSH, LH, oestrogen, and progesterone.
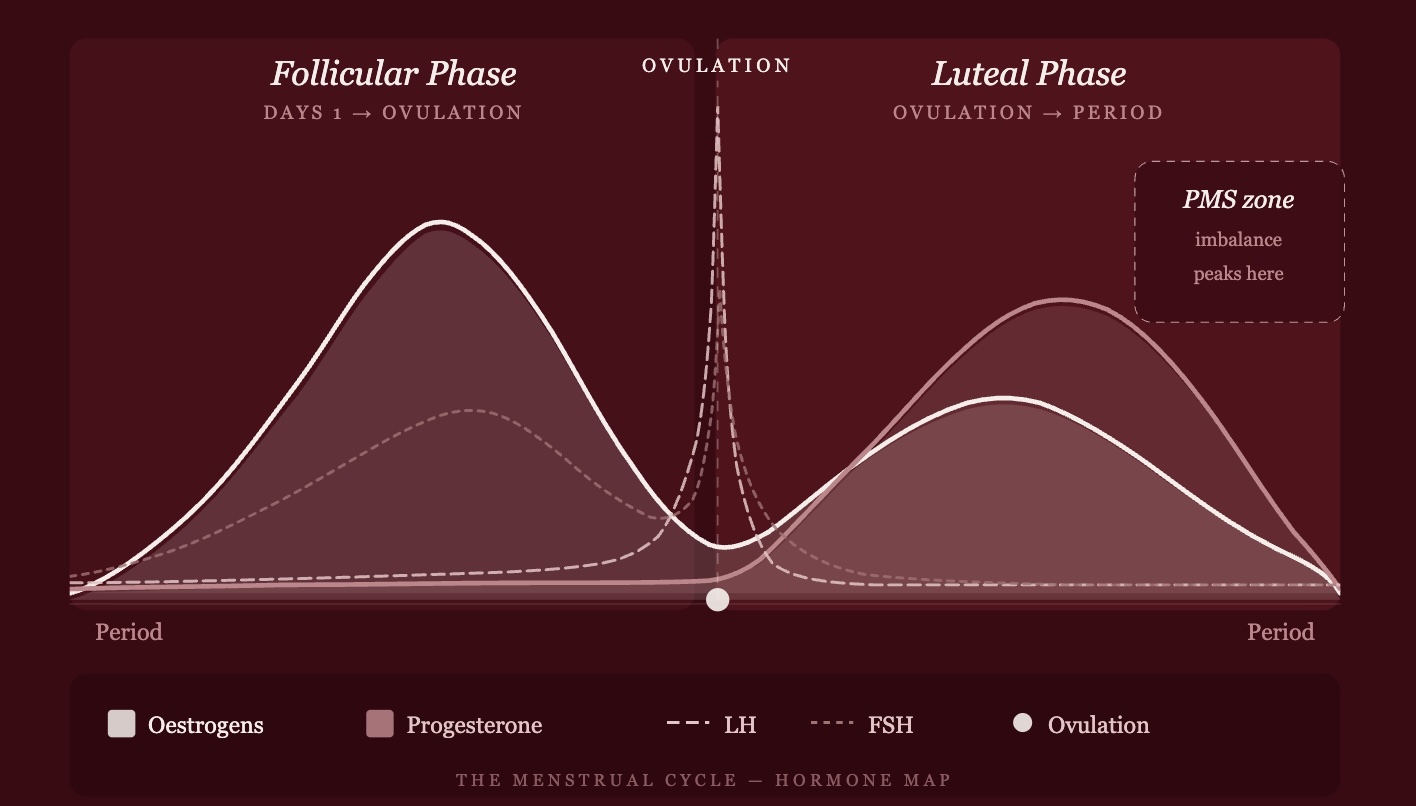
What causes PMS?
The exact cause isn't fully understood, but research points to several interconnected factors:

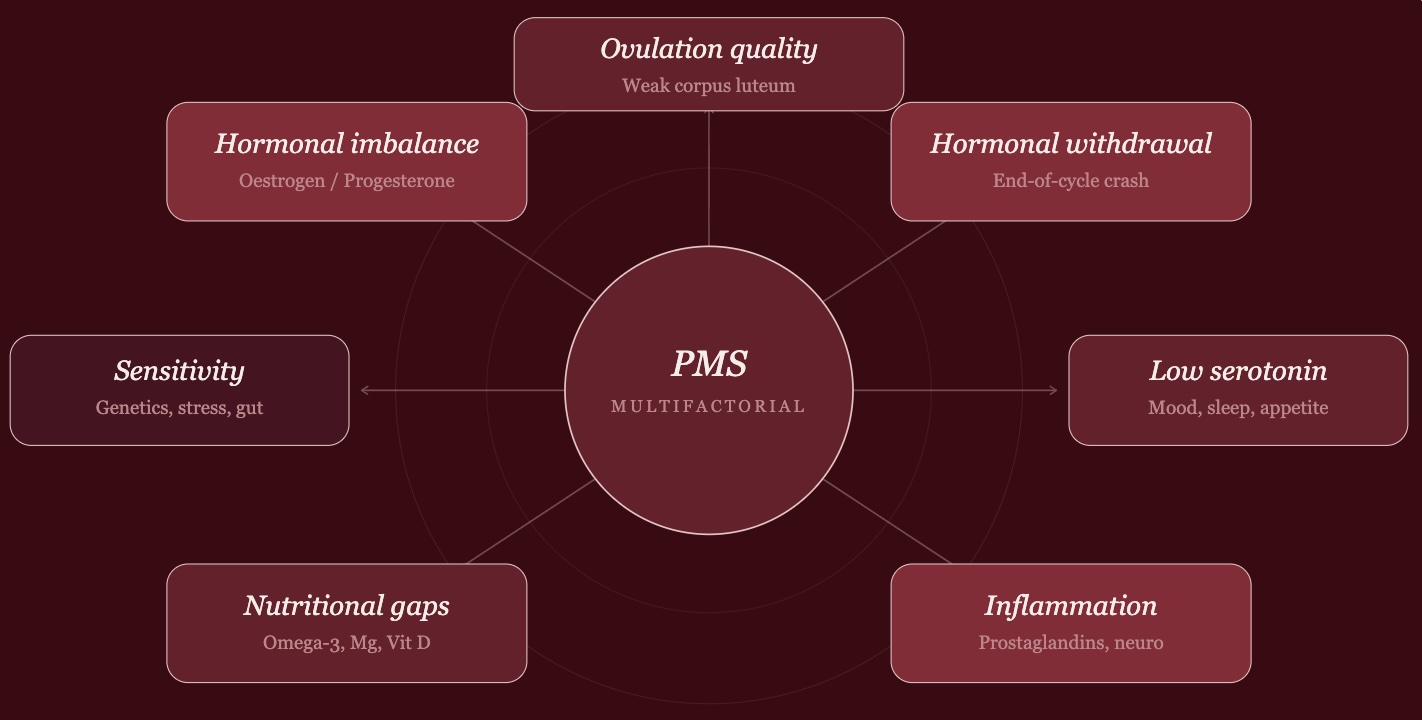
A closer look: oestrogen dominance
After ovulation, oestrogen should take a back seat while progesterone rises. But in oestrogen dominance, this balance is disrupted in one of two ways:
True oestrogen dominance: Oestrogen levels remain too high, often because the body isn't clearing used oestrogen efficiently, or due to exposure to environmental oestrogens (xenoestrogens from plastics, cosmetics, etc.)
Relative oestrogen dominance: Oestrogen levels are technically fine, but progesterone production is too weak — often due to poor quality ovulation. The ratio is off.
In both cases, progesterone — the calming, muscle-relaxing hormone — can't do its job properly.


How is PMS diagnosed?
There's no single test for PMS. Because symptoms vary so widely between individuals, diagnosis is primarily clinical and based on pattern recognition. The most useful tool? A symptom diary.
Track your symptoms daily for at least two cycles, noting when they appear and when they disappear. If they reliably peak in the 5–14 days before your period and resolve once bleeding begins, that's a strong indicator of PMS.
Your doctor may also order a blood test around day 21 of your cycle (7 days after ovulation) to check your progesterone level — ideally at its peak — as well as oestrogen levels.
Treatments & lifestyle approaches
Medical options
Medical treatments aim to manage symptoms rather than resolve the underlying cause. Options include:
The contraceptive pill — pauses the natural cycle and can reduce PMS. But it masks symptoms rather than treating them, and some people still experience a hormonal-withdrawal PMS around the pill break.
SSRIs (antidepressants) — can relieve mood-related symptoms. Again, more of a support tool than a root-cause fix.
Progesterone supplementation — bio-identical progesterone (Utrogestan, Prometrium) or synthetic (Duphaston) taken after confirmed ovulation for ~10 days. Addresses the deficiency directly.
Pain relief — anti-inflammatory drugs (NSAIDs) can help with physical pain by reducing prostaglandin activity.
Lifestyle & natural approaches
These are the approaches with the most sustainable, long-term impact — and where even conventional doctors tend to agree:
Sleep — chronically poor sleep worsens every PMS symptom. Aim for 7–9 hours, especially in the luteal phase.
Anti-inflammatory diet — prioritise vegetables, fruits, omega-3 rich foods (salmon, walnuts, flaxseed), and reduce ultra-processed foods, alcohol, and refined sugar.
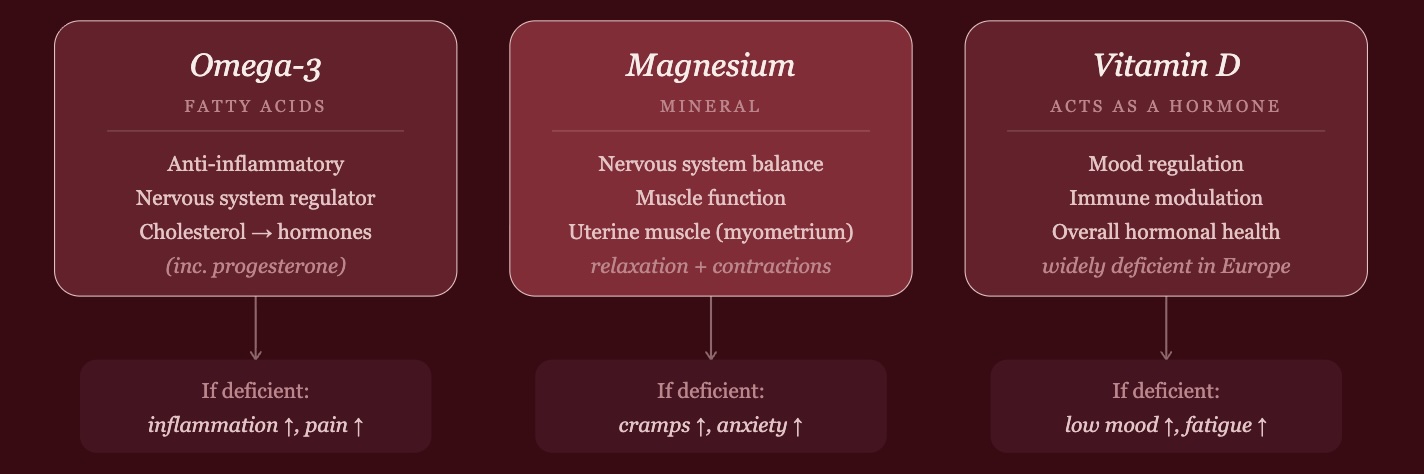
Key supplements — magnesium (for cramps and mood), vitamin D, omega-3, and herbal remedies like vitex (chaste tree berry) and evening primrose oil show promising evidence.
Exercise — regular movement releases endorphins, reduces inflammation, and eases pelvic tension. Gentle yoga or walking during the luteal phase can be particularly helpful.
Stress reduction — chronic stress depletes progesterone and worsens hormonal imbalances. Mindfulness, breathwork, or simply protecting your rest time matters
Understanding PMS isn't about labelling your worst days — it's about learning your body's signals. When you know what's happening hormonally and why, you can meet yourself with more compassion, and make informed choices about how to feel better.
Every body is different. If your symptoms significantly affect your quality of life, a conversation with a hormone-informed healthcare professional is always worth it.