- Mar 24
How I Reversed My 5-Year-Old's Psoriasis — Naturally
- Shabina
- Skincare, Postpartum & Kids' health
- 0 comments
No steroids. No harsh creams. No "just wait and see." Just a stubborn mum, a lot of research, and a whole lot of trust in the body's ability to heal itself.
Let me paint you a picture. You're moving country, you've just uprooted your entire life, your little boy is adjusting to all kinds of changes — and then one morning, you notice patches on their skin that look… wrong.
Not the usual dry skin wrong. Something-is-going-on wrong.
That's where my story starts. And if you're reading this with a knot in your stomach because your own child has mysterious skin issues that no one seems to take seriously — first: I see you.
Second: keep reading.
I've had eczema since I was a teenager. The kind that flares at the worst possible moments — exam season, job interviews, public gatherings... My arms, my neck, my elbows, my eyes. I tried the steroid creams, of course. Everyone does. And every single time, the skin would calm down briefly… only to come back angrier than before the moment I stopped.
I eventually figured out that steroids were playing whack-a-mole with my symptoms while ignoring whatever was actually causing them. They didn't fix anything — they just temporarily quieted my skin down, like turning off the smoke alarm without dealing with the fire.

So when my 5-year-old son started developing strange red, scaly patches on his scalp after we'd moved, I was already primed to think differently.
I knew what the conventional playbook looked like. And I wanted to write a different one for him.
You're not alone — the numbers are staggering
Before we go further, let's talk about scale. Because one of the loneliest feelings in this journey is thinking you're the only one navigating this. You're not. Not even close.

Psoriasis in children is less common than in adults, but it's rising. In Western Europe and high-income countries, the numbers are climbing. And crucially — most of these children are being handed the same prescription: steroid cream, follow up in six months. Many parents know, in their gut, that there has to be more to it.
Genetics got you here. Epigenetics can get you out.
Yes, there's a genetic component to both eczema and psoriasis. If you or a close family member has either condition, your child is at higher risk. That's just biology.
But here's what I find genuinely exciting: epigenetics. This is the science of how your environment, lifestyle, stress levels, diet, and emotional state can switch genes on or off — without changing the DNA itself. You may have inherited the predisposition. But genes need triggers to express themselves.

For our son, the timing was not a coincidence. The psoriasis appeared during our move to a different country — a big, disorienting life upheaval for a small person who had no say in the matter. New country. New friends. No familiar faces. His nervous system was under stress, and his skin was sending up the signal flares.

Step 1: Getting a proper diagnosis
want to be honest with you about the medical journey, because it wasn't smooth, and I suspect yours might not be either.
When I first brought my son to our new paediatrician, she glanced at his scalp and said — rather dismissively — "oh, that's just cradle cap" . My son was five years old. Cradle cap. At five. Are you kidding me ?
I smiled politely, thanked her, walked home, and then spent the next 45 minutes rage-googling images of cradle cap and arriving at the very obvious conclusion that this was absolutely not cradle cap.
I went back. I was kind, but I was persistent. I explained that I had personal experience with inflammatory skin conditions, that the patches had a very specific appearance, and that I needed a referral to a dermatologist. She agreed, somewhat reluctantly.
The dermatologist was… not the warm, holistic, root-cause practitioner of my dreams. She was efficient, confident, and had a prescription pad at the ready before she'd finished examining him. Topical steroids. "Standard protocol."
I asked about alternatives. I asked about nutrition. I asked about vitamin D, about inflammation markers, about the role of stress. She looked at me the way only a certain type of specialist can look at a questioning parent — like I'd asked her whether the moon was made of cheese.
But she had given me what I needed: a confirmed diagnosis of psoriasis. And with a clear diagnosis in hand, I could finally start doing the work I actually wanted to do.

Step 2: Testing — actually understanding what's going on inside
Once I had the diagnosis, I didn't just want to suppress the symptoms. I wanted to understand the terrain. Why was his immune system misfiring? What was the body missing? What was it being overwhelmed by?
We did a thorough round of functional testing — not all of it through the conventional GP, I'll be honest. Some of it through naturopathic and kinesiology practitioners I genuinely trusted.
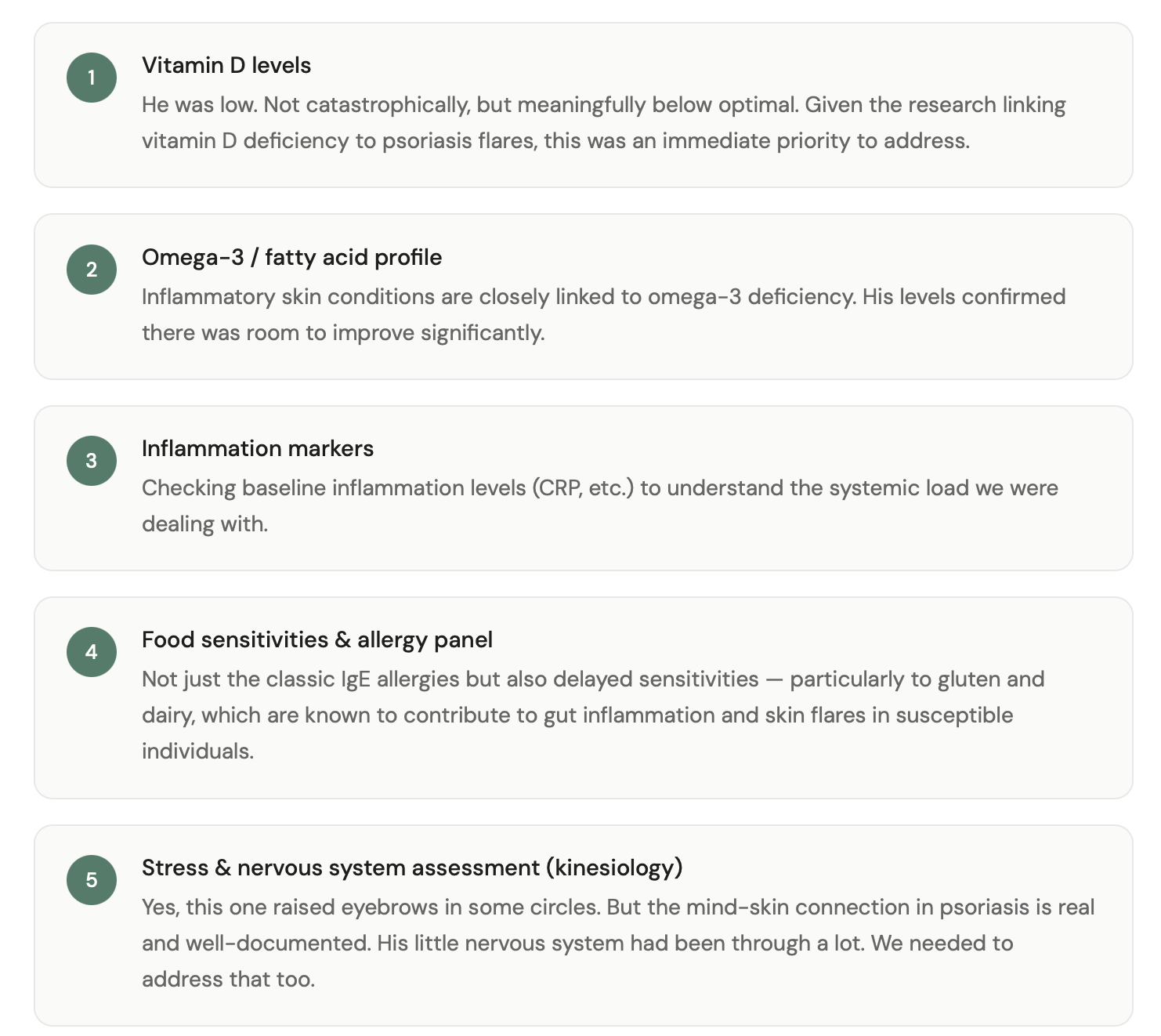
Step 3: The holistic protocol that actually worked
This is the part where I want to be very clear: this wasn't a single magic fix. It was a multi-layered approach, applied consistently over several months, guided by practitioners I trusted. If you're looking for a quick solution, I'm sorry — I don't have one. But if you're willing to think systemically and play the long game? It's absolutely worth it.

The nutrition piece — and why gluten and dairy matter
I want to address this head on, because "go gluten-free" gets eye-rolls in certain circles. We didn't do this because it's fashionable. We did it because of what happens at a gut level with inflammatory skin conditions.
In genetically susceptible individuals, gluten and dairy proteins can increase intestinal permeability (sometimes called "leaky gut"), allowing inflammatory particles into the bloodstream that then drive immune reactivity — including in the skin. The psoriasis-gut connection is increasingly recognised in dermatology research, even if it hasn't fully made it into standard clinic protocols yet.
We were strict for 12 weeks, then reintroduced slowly. Every child is different. That's the point of testing and observing rather than following a one-size-fits-all script.
The emotional piece — the one everyone underestimates
Psoriasis is not just a skin disease. The research is clear: there is a deep, bidirectional connection between psychological stress and psoriasis. Stress triggers flares. Flares cause stress. It's a loop, and in children who have no sophisticated tools for processing big emotions, that loop can spin quickly.
For our son, the move had been massive. He had lost his friends, his familiar spaces, his language comfort zone. He was brave and adaptable on the outside. Inside, his nervous system was telling a different story — and his skin was the translator.
We worked on safety, predictability, connection. More one-on-one time. Less rushing. Creating new rituals. Kinesiology sessions that helped release some of the somatic tension he was holding. It sounds soft. It was some of the most powerful medicine in our toolkit.
Patience is genuinely part of the protocol
I won't pretend it was fast. The goal was never to find a cure or a quick fix. It was to create the conditions in which his body could heal itself. And it did. But it takes time.
Where we are now
Once the psoriasis is completely healed on the surface, don't just stop there. Prevention is key.
We don't wait for the next flare up.
Winter means extra vitamin D and omega-3. Stressful periods (school transitions, family upheaval) mean extra emotional support and a return to cleaner eating. We know the triggers. We work with his body, not against it.
What I want you to take away
If your child has been diagnosed with psoriasis — or if you're still fighting to get that diagnosis taken seriously — here's my honest advice:
Trust your gut. You know your child's skin better than anyone. If something feels wrong, push for clarity. Harass the paediatrician (nicely). Get the referral. Get the diagnosis. You need that baseline.
Look upstream. Ask why. What could be driving the inflammation? What's happening in the gut? What's happening emotionally? Skin symptoms are rarely about the skin alone.
Assemble your team with intention. Your GP and dermatologist for diagnosis and monitoring. A naturopath or functional medicine doctor for root cause. A kinesiologist or therapist for the emotional dimension. You don't have to choose between conventional and holistic — you can use both.
Give it time. The body didn't get inflamed overnight, and it won't heal overnight either. Expect months, not weeks. But the improvements along the way will keep you going.
PS : You've got this. Your child is lucky to have someone who cares this much (and this article was looong so celebrate yourself). 💚